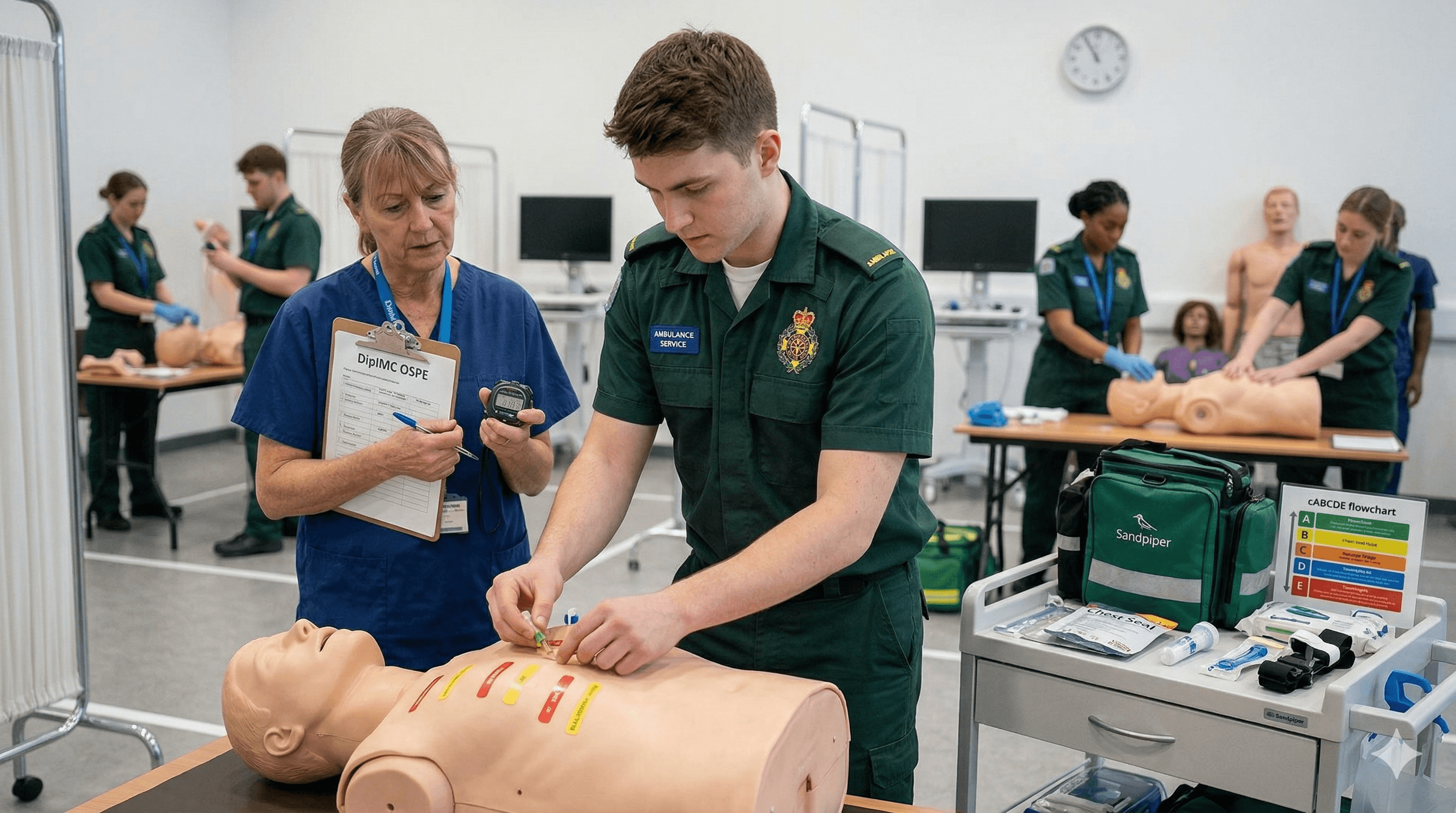
The DipIMC OSPE is a practical examination. Reading about thoracostomy is not the same as performing one on a mannequin with an examiner watching and a timer running. Reading about triage is not the same as triaging five simulated casualties in 8 minutes.
OSPE preparation requires practice, not just study. This resource provides structured guidance for each major OSPE station type.
Trauma Station Walkthrough
Approach: cABCDE is your framework. Every trauma station starts here. Verbalise each step: "I am approaching the patient. The scene is safe. I am assessing for catastrophic haemorrhage..." State your findings out loud — the examiner marks what you say.
Catastrophic haemorrhage: Identify the source. Apply direct pressure, tourniquet, or wound packing as appropriate. State what you are doing and why. Do not move to A until C (catastrophic) is controlled.
Airway with C-spine: Assess patency while maintaining manual in-line stabilisation. State your airway findings. Intervene if needed (jaw thrust, OPA, NPA, intubation or surgical airway if indicated).
Breathing: Look, listen, feel. Respiratory rate, SpO2, chest movement symmetry, percussion, auscultation. Identify tension pneumothorax, open pneumothorax, flail chest, haemothorax. Intervene as indicated (chest seal, thoracostomy, needle decompression).
Circulation: Pulse, BP, capillary refill. Identify shock. IV/IO access. Fluid resuscitation. Pelvic binder if indicated. State your fluid strategy.
Disability: GCS, pupils, blood glucose, lateralising signs. Brief neurological assessment.
Exposure: Maintain temperature control. Log roll for posterior examination. Complete secondary survey if time allows.
Procedural Skills Stations
Needle thoracostomy/finger thoracostomy: Know the indications (tension pneumothorax), the landmarks (2nd intercostal space mid-clavicular or 4th/5th intercostal space anterior axillary line), and the technique. Practise on a mannequin.
Surgical airway: Front-of-neck access for "can't intubate, can't oxygenate" emergencies. Know the landmarks (cricothyroid membrane), the technique, and the equipment. Practise until the technique is smooth and confident.
Tourniquet application: High and tight, proximal to the wound. Note the time. State the indication. This should take under 30 seconds.
Pelvic binder application: Identify the suspected pelvic fracture. Apply the binder at the level of the greater trochanters. State the indication and the technique.
Communication Station Walkthrough
Handover to receiving hospital: Use a structured framework (ATMIST or similar): Age, Time of incident, Mechanism, Injuries found, Signs and symptoms, Treatment given. Be concise, clear, and structured. The examiner is marking your communication quality, not the length of your report.
Breaking bad news in the field: A bystander asks about their loved one who has died at the scene. Use SPIKES. Be direct but compassionate. Allow silence. Respond to emotions before moving to practicalities.
How to Practise
Simulate stations with colleagues. Use equipment from your clinical workplace. Time yourself. Give and receive structured feedback. Record your performance and review it.
Build the clinical knowledge that underpins every station with the iatroX DipIMC Q-Bank. Develop structured clinical reasoning with Brainstorm. Verify management pathways with Ask iatroX. The knowledge and the practical skills together produce the OSPE performance the examiners reward.